
Health evaluations typically begin with blood work, imaging, or the assessment of specific symptoms. But one of the richest signals of health is something much more fundamental: how people move.
Mobility reflects far more than whether someone is active. It reflects strength, pain, balance, coordination, neurological control, recovery, and resilience. Clinicians intuitively recognize these signals just by watching someone walk and can tell whether they seem strong, fatigued, unstable, or unwell.
And yet, healthcare still measures mobility poorly.
In most settings, mobility is assessed only episodically, during a clinic visit, a structured test, or a subjective observation. Those moments can be useful, but they capture only a small part of how people actually function in daily life. The limitation is not only the short duration of measurement, but also the artificial setting. Understanding how people move in their own environment is often more informative clinically, and it is now technically feasible without requiring continuous 24/7 monitoring.
This gap matters because mobility is not a niche concern limited to older adults or people undergoing rehabilitation. It is a broad and meaningful expression of health across adulthood.
One reason mobility remains underappreciated is that it is often associated only with frailty or advanced disease.
But the reality is broader.
Mobility changes for many reasons across the entire adult lifespan. Sometimes the main driver is pain. Sometimes it is weakness. Sometimes it is balance, sensation, or higher-level motor control. These patterns often overlap in the same person, and together they shape how someone functions in the real world.
The figure below offers a schematic view of that broader picture. It is not meant as a precise prevalence breakdown, but as a summary of how different mobility patterns contribute across adulthood.
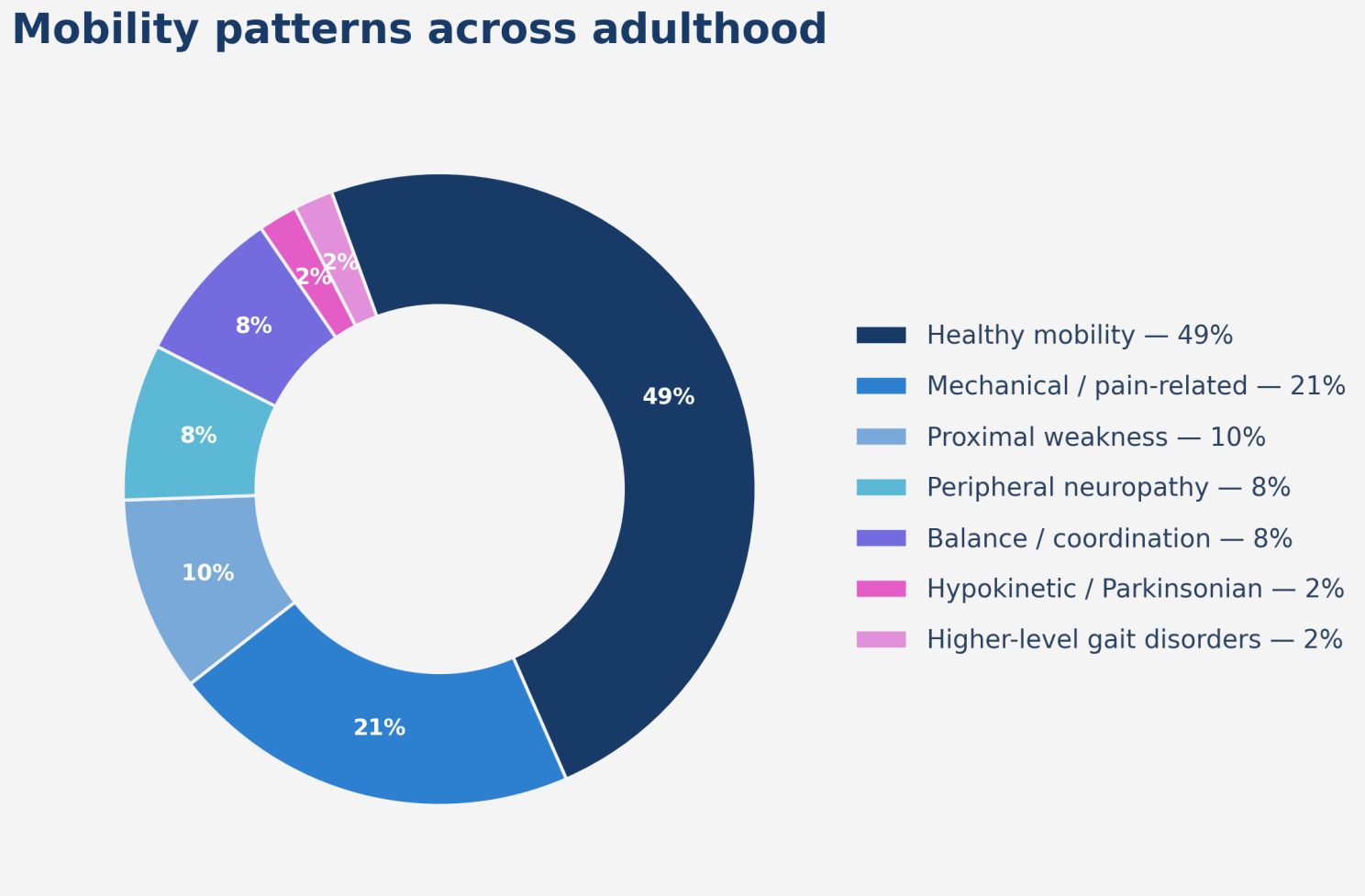
What this figure highlights is simple but important: non-healthy mobility is not a marginal phenomenon.
Mobility limitations affect adults across the lifespan, and they arise from multiple overlapping physiological and clinical processes. That is what makes mobility such a rich and general signal of health.
Changes in gait and function are associated with fall risk, hospitalization, loss of independence, disease progression, and recovery after treatment. Gait speed, in particular, is widely recognized as the “sixth vital sign” and is strongly associated with fall risk, hospitalization, and functional independence.
But gait speed alone is not enough. People may have the same walking speed while differing substantially in stability, asymmetry, coordination, or movement quality. Understanding real-world health and function requires moving beyond single summary measures toward a more complete view of mobility.
Gait and mobility contain structure: speed, rhythm, symmetry, variability, coordination, and postural control. These characteristics can reveal meaningful differences in health, long before they are observed in the clinic. This is especially important as healthcare shifts toward function, outcomes, and value.
Humans are naturally good at sensing meaning in movement and notice when someone looks unstable, slower, weaker, or less confident. The challenge now is to turn those impressions into measurements that are objective, continuous, and clinically interpretable.
That is where digital mobility measurement becomes important.
The opportunity is not simply to collect more data. It is to measure function in a way that reflects real life, captures meaningful change over time, and supports better clinical understanding.
For many years, the main barrier was not conceptual. It was practical.
While the clinical importance of mobility has long been recognized, measuring it outside gait labs or structured clinical settings was difficult. That is now changing.
A broader community is forming around digital mobility outcomes, including researchers, clinicians, industry, and initiatives such as Mobilise-D. Progress in this field will require more than sensors and algorithms. It will require validation, clinically interpretable measures, and evidence from real-world settings. This is not something a single company or algorithm can define on its own. It requires a field.
Mobility is one of the richest signals of human health because it reflects the body as an integrated system. It expresses pain, weakness, balance, neurological control, recovery, and decline, often all at once.
Blood pressure, glucose, and cardiac rhythm are already established as sources of continuous physiological insight. Mobility deserves similar clinical attention. It reflects the integrated output of multiple systems and captures something healthcare often misses: how people actually function in the real world.
Healthcare should treat mobility as a core signal of health because function is too important to leave to occasional observation alone, and it can now be measured continuously.
The future of healthcare will depend not only on measuring disease, but on measuring how people actually function in the real world.
And mobility is one of the clearest ways to do that.
This piece was originally authored by Yuval Naveh, Co-Founder & Chief Scientific Officer at OneStep, and shared via LinkedIn, where he discusses the intersection of digital health and human mobility.